27th November 2014 marked a significant date for the NHS (in England?). The duty of candour came into force. The duty legally obliges hospitals to inform patients when mistakes have been made and the patients have experienced moderate or significant harm, whether a complaint has been made. The duty of candour applies to all NHS trusts and is regulated by the Care Quality Commission ("CQC"). Failure to comply can be a criminal offence and a person can be liable and can result in conviction or a fine.
The duty of candour was one of the recommendations made by the Francis Report in order to improve the level of patient care. The preparation of the Francis Report in the first instance was motivated by the Mid Staffordshire NHS Foundation Trust scandal.
The Secretary of State for Health has said that the duty of candour will better hospital standards and patient care by recognising mistakes, which will in turn allow procedures to be devised to lessen the probability of identical errors occurring again. He considers that a significant percentage of preventable harm and deaths can be decreased by requiring the NHS to be honest and open about mistakes made.
How does it operate?
The Health & Social Care Act 2008 (Regulated Activities) Regulations 2014 outlined how the Duty of Candour will work.
The Duty of Candour occurs in the event of a "notifiable safety incident". In other words, when one of the following events arises:
(i) The death of a patient, so long as the death is in relation to the mistake, as oppose to expected path of the underlying condition.
(ii) Severe harm or moderate harm to the patient.
Once realised that the notifiable safety incident has occurred, notification must be given to the patient, or their family as soon as is practicable. The notification must:
- be given in writing;
- provide a truthful account of all the facts;
- if possible, agree what further enquiries are appropriate, and again if possible;
- include an apology.
All information directly relating to the incident must be given and reasonable support must be provided.
Will the duty of candour cause an increase in clinical negligence claims?
One must remember that these regulations came around, largely, from Sir Robert Francis QC's inquiry into the healthcare provided in Mid Staffordshire. Accordingly, the duty of candour holds the aim of improving healthcare. If that happens, then of course, there will consequently be less clinical negligence claims.
Additionally, the Duty of Candour aims to achieve cultural change. These guidelines seek to generate a setting where medical professionals are not afraid to discuss mistakes, thus allowing us to learn from mistakes. When errors are made, then medical staff shall be urged to engage with patients and most importantly, be open about what went wrong.
Finally, the regulations do not make any reference to civil liability. In this context, on the contrary to the health and safety regulations used in the workplace, a notifiable safety incident, and a subsequent report, will not automatically give rise to a successful compensation claim.
As such, ultimately, the duty of candour is not designed to assist harmed patients to succeed in claims for compensation but rather, the duty of candour seeks to prevent new litigation
Speaking as an active clinical negligence lawyer, I only welcome the duty of candour. The NHS has to start somewhere, and this certainly is a step in the right direction. More often than not, prospective clients get in touch with us, not only because something has gone wrong but because they are not able to obtain an explanation from the medical professionals involved. I only hope that the regulations, and their guidelines, will be thoroughly complied with.
Should you have any concerns in respect of the care and treatment received, and/or, if you seek advice about your right to complain and, the Duty of Candour, then do contact our devoted Clinical Negligence Team on 01633 262 848.
Clinical Negligence
Caesarean Section ("C-Section"). Despite the potential associated injuries, the number of C Sections are on the rise which is causing a stir in the medical world
What is a C-Section
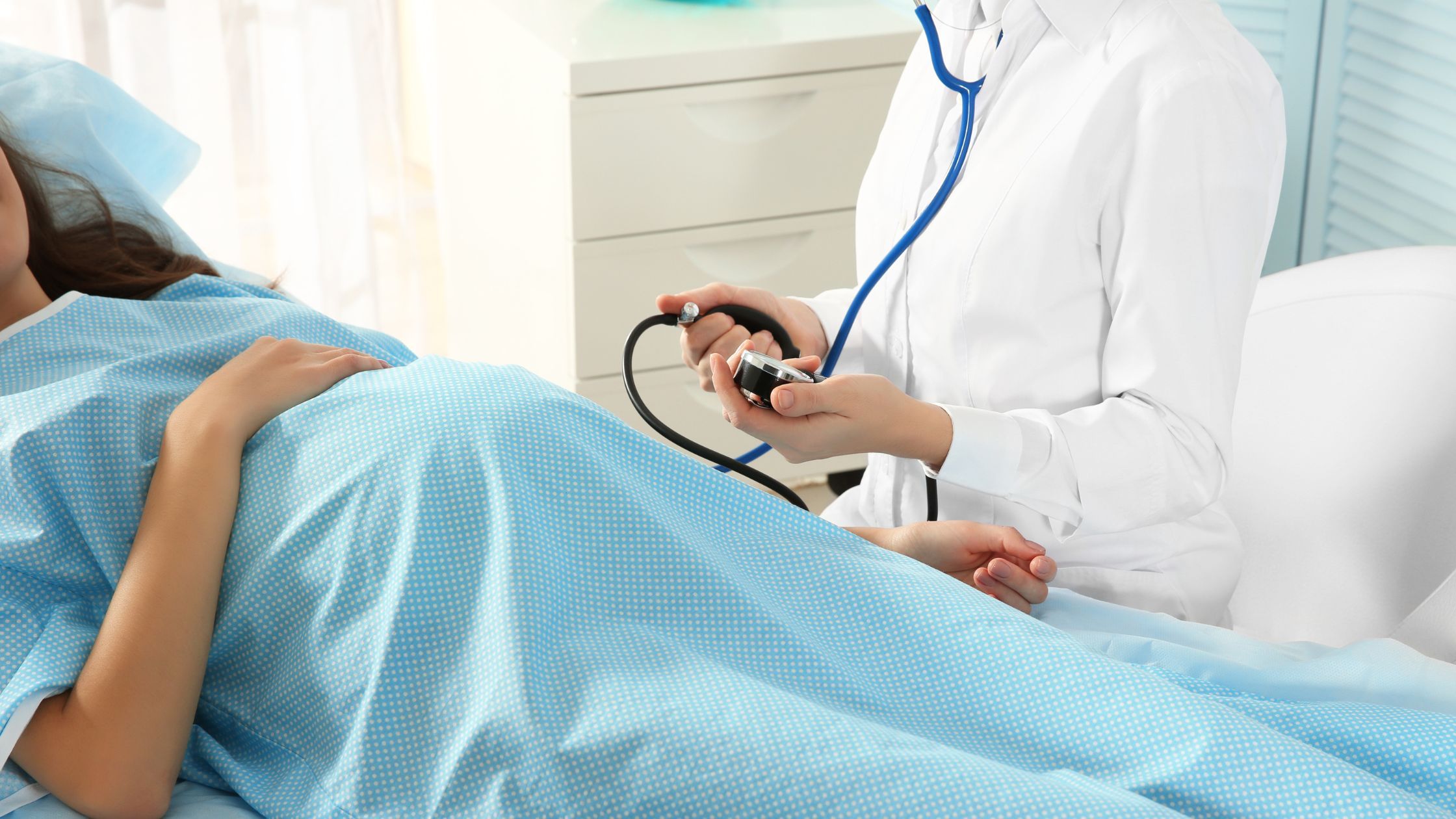
As the result of an obstetric emergency or on the infrequent occasion, the mother's choice, a C-Section is performed. A C-Section involves making an incision at the front wall of a woman's abdomen through to her uterus and thereafter the baby is removed.
Examples of reasons for C-Section:-
- Obstetric emergency;
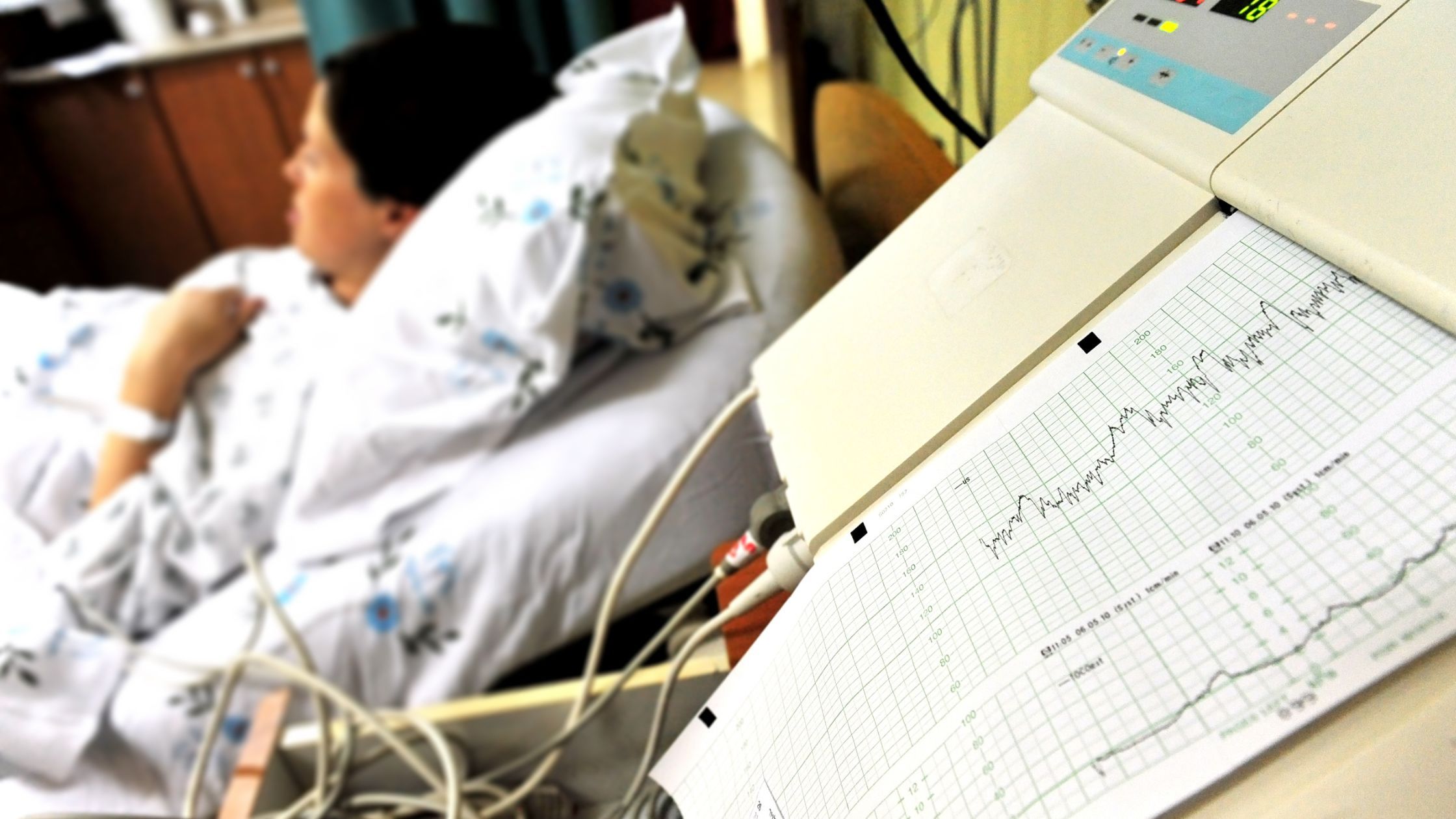
There are a number of obstetric emergencies which may require a C-Section to be carried out. The most common causes are: fetal distress during labour (shown by either accelerated or decelerated heart rate); abruption of the placenta; the position of the baby not being ready for vaginal delivery (such as being in breach); failed attempts of forceps or ventouse assisted delivery and, cord prolapse.
- An increase in older first-time mothers.
- An increase in the number of women suffering from obesity.
- Women requesting the procedure
Reasons for the increase
There has been a sharp rise in the number of babies being born by C-Section.
While the majority of women continue to deliver their babies vaginally, there has been a steep increase in babies born by caesarean. In the 1980s, it was only about 1 in 10 births and now that proportion is 1 in 4.
There are a number of reasons for the increase.
- More obese women giving birth
- Older first-time mothers
- Fear of delivery which increases stress hormones and can inhibit a more straightforward labour
- A small number of mothers asking for the procedure
An increasing fear of litigation